Buff Muff Method™ vs Restore Your Core®

If you're leaking when you laugh, running to the bathroom urgently and/or frequently, dealing with prolapse symptoms, or struggling with low back pain, pelvic pain, or painful sex, you've probably started searching for answers.
Two programs you may hav...
I don’t know about you but my day can not really begin until I have had a poop. Not just any poop but a #4 poop on the #2 chart. If you don’t know what I am talking about stay tuned. In this article we will look at what constipation is, why it can happen, how we can tell if we are constipated (it...
In the realm of fitness and wellness, creatine monohydrate has long been celebrated as a powerful supplement for enhancing strength, muscle mass, and overall athletic performance. However, its benefits for women have often been overshadowed or misunderstood. Contrary to common misconceptions, cre...
Disclaimer: I am not a doctor or a hormone specialist. I am nearing completion of my Menopause Support Practitioner Certification and am post-menopause myself. I follow the evidence and look to vocal advocates for female sexual health and wellness like Dr Kelly Casperson and Dr Rachel Rubin. Thi...
Electrical stimulation (e-stim) of the pelvic floor muscles is often used in clinic or at home to help improve incontinence and prolapse symptoms. Pelvic floor muscles are an essential part of our body that provide support to the bladder, bowel, and uterus. When the pelvic floor muscles are not work...
The best description of the vagina in menopause is that it can go from a pleated skirt to a pencil skirt. I have heard this from Michelle Lyons of Celebrate Muliebrity and Julia Di Paolo, Reg. PT of PhysioExcellence
Our Vagina
We have folds in the walls of the vagina called Rugae that can thin as ...
What can I do about Tailbone Pain?
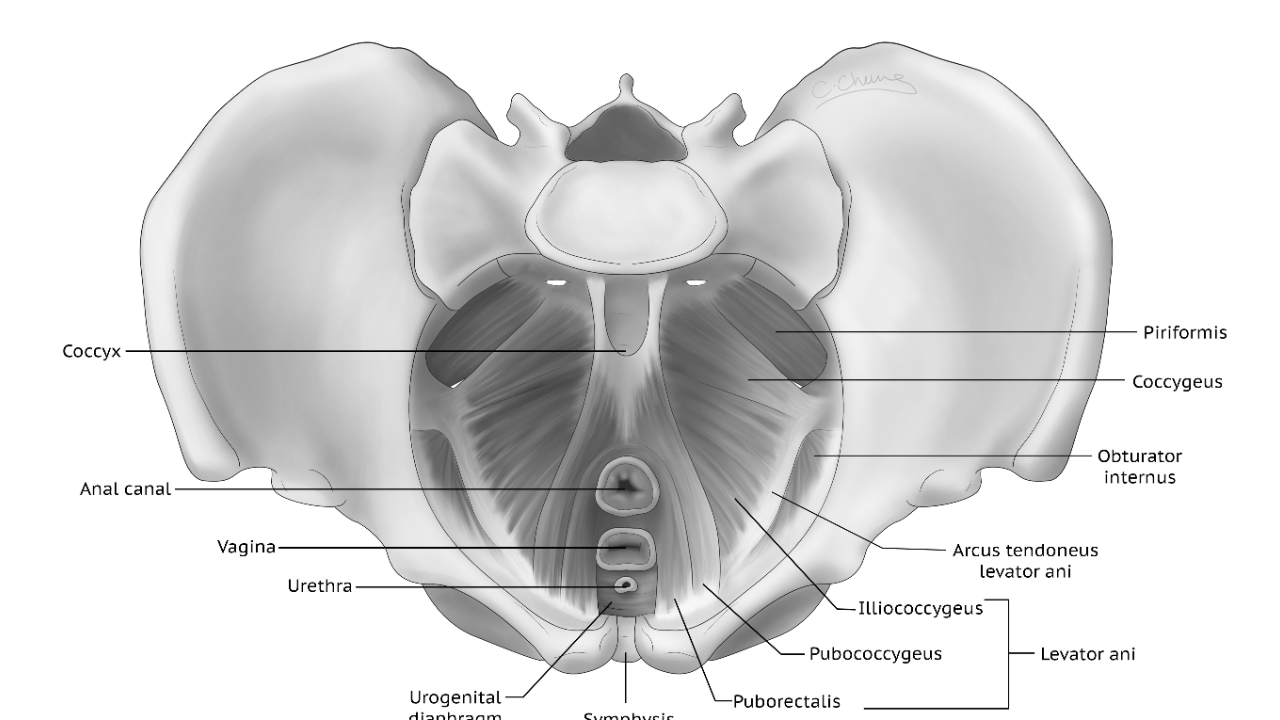
The tailbone or coccyx is a non-functional tail in the human body. It is located at the bottom of the spine and is one of the attachment points for the pelvic floor muscles. Tension in the pelvic floor, childbirth, falls on the tailbone, and even sitting posture c...
We live in an on-the-go society, and our smartphones have apps for pretty much all our wants and needs, from fashion, food and sleep, to fitness and exercise programs.
I launched my Buff Muff App a little over a year ago and am very excited at the response. Women can now carry their very own person...
I have been thinking about it for a couple of years and decided to go for it. I love chatting with people about all things pelvic health. Conversations between two lips, so to speak.
We officially started our first episode on Jan 17th, telling my story, and we record a new episode weekly. The infor...
It can be a struggle in our daily life when we suffer from Rectocele Prolapse.
A rectocele happens when the rectum falls forward into the back of the vagina. The tissue becomes thin and weak over time between the rectum and the vagina, resulting in a rectocele.
Symptoms of Rectocele Prolapse
You...